Essential life functions, breathing, eating and communication all happen in the upper airway, every single day and night, and we do not even think about them ; breathing, eating and communication. They just happen right?
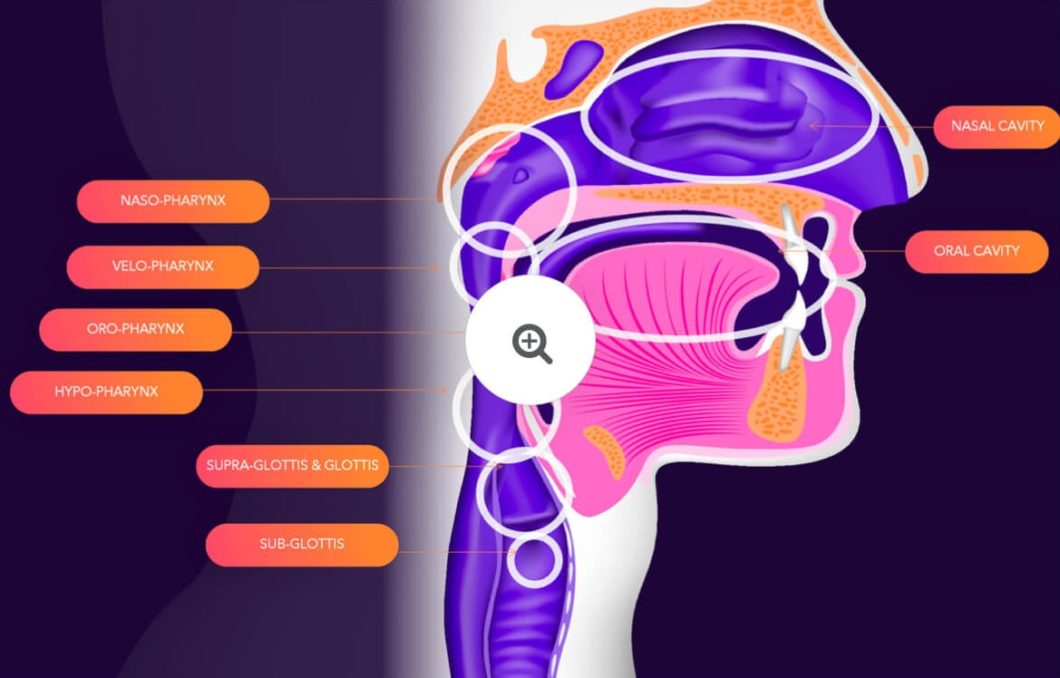
In a nutshell, the upper airway begins at the front of the face and extends just beyond your larynx (voice box). this zone. Mostly people are unaware, that is, until something goes wrong.
When things go wrong there is a medical name for it, you might hear words like, dysphagia, dysphonia, chronic cough, dysfunctional breathing, speech disorder, snoring, mouth breathing or obstructive sleep apnoea, to name a few!
You may be even be wondering, what is the upper airway, what does that mean?
“ I don’t know how many times I have heard from patients that they never realised how important voice was, until they lost it.”
“More recently, advances sleep medicine recognise the role of airway for good quality sleep at night, & hails a new era and new role for myofunctional science and practice in medicine.”
-Sharon Moore
Who needs help with a disorder of the upper airway?
Your Medical Specialist, Dentist, Orthodontist, may have referred you, because they have already formed an opinion that you would benefit from an upper airway assessment and treatment program. Best results occur with a team effort. Early detection and treatment is ideal but therapy can occur at any age.
Common reasons for referral:
- “no matter how much sleep I get, I still wake tired”
“I started snoring” - “Ellie wants her braces off for the school formal, but the Orthodontist said not until the tongue thrust is fixed”
- “My throat tightens a lot when I am near strong smells like perfume, or paint, sometimes it’s so tight I can’t swallow or speak.”
- “I have to clear my throat and cough all day, it barely stops, there’s always irritation in the throat.”
- “My son is a restless sleeper, every morning it looks like a hurricane went through his bed overnight, then he acts like a hurricane all day.”
- “Allergies seem to run in the family and so do snotty noses, we all have to mouth breathe.”
- “His breathing at night sounds like a freight train, but he’s not snoring, does that mean he is a deep sleeper?”
- “my son is 6 and still has a dummy at night and it is wrecking his teeth”
- “Johnny had his tonsils and adenoids out, he was ok for awhile but his sleep apnoea and snoring has started again”
- “My son yells all day and often loses his voice, the ENT says he has nodules, is that bad?
- “I noticed after the tonsils were taken out that my daughter had really nasal speech”.
- “Katy, still chews with her mouth open, no matter how much we remind her.”
- “Michael is 3 years old and has low muscle tone with saliva control problems”
- “Samuel is a mouth breather and his mouth is always open”
- “Dion’s had 12 months of traditional Speech Pathology technique and nothing has changed.”
How do I make an appointment?
If you have been referred to Well Spoken by your medical or dental specialist click here.