Sleep health: unrecognised under-rated underdone
Sleep is a global health challenge, which is why all health professionals should screen every person for sleep health and sleep disorders. I believe we have an imperative to educate far and wide about the consequences of untreated sleep problems. Here we are talking not just about sleep disorders but simply unhealthy sleep habits that undermine good sleep. At Well Spoken we screen every patient for sleep and sleep-breathing issues, frequently encountering families whose children have disrupted sleep, wake frequently or consistently, have signs of insomnia, wake unrefreshed, have nightmares, wet the bed and more. Alongside this, many parents are wading through daily life on insufficient sleep.
Yet many parents say, in the face of these reported sleep behaviors, they think their child is getting good sleep, despite accompanying daytime ‘shenanigans’. They feel confident that if their child spends the right number of hours in bed, their sleep must be sufficient. Meanwhile, others acknowledge worrying sleep and daytime behaviors but dismiss these as part of the norm when raising kids.
Why is this so? Sleep myths and misperceptions persist among both the public and professionals alike, interfering with sleep health being taken seriously, with many believing that poor sleep is to be endured in the trenches of parenting.
It does not need to be this way. Any signs of sub-optimal sleep beg the big question: Why?
Breathing during sleep really matters
We know that up to 40% sleep problems can be resolved at home simply by setting up a great sleep environment, having great routines around bed-time. But what happens when this does not work? We need to dig deeper and find out why. In children, sleep and breathing issues are common. ‘Dysfunctional’ breathing during sleep requires the body to ‘work harder to breathe’ potentially interfering with good sleep quality and architecture. At Well Spoken we look closely at breathing during sleep and any sign of audible breathing. While snoring and mouth breathing often aren’t seen as serious issues by parents and even some health professionals, the truth is that any breathing difficulties will lead to disruption of the sleep architecture that is fundamental to the brain cleansing and restoration (glymphatics) that must happen every single night for the brain to fully restore and regenerate to be ready for the next day. This then leads to a range of developmental delays and behavioural consequences, that we refer to as ‘shenanigans’. It’s not your child’s fault.

It’s not just about oxygen
Breathing issues activate the sympathetic nervous system i.e. rev up the body rather than relax it. This in turn disrupts sleep architecture keeping children in a lighter sleep phase which fragments sleep and may be the very reason why kids wake at night. Kids with these problems can suffer the same daytime physical, mental, emotional and social consequences as a child with a more serious night time breathing issue like sleep apnoea, but they may be misdiagnosed as having anxiety or ADHD, oppositional defiance, depression, autism, PTSD, aggression, emotional fragility, or learning problems. They may wet the bed or have unexplained waking and the wrong treatment may be prescribed. If the problem is due to imperfect breathing during sleep, no amount of psychological support, bells, whistles or pharmaceuticals will fix this problem. Fixing the airway and breathing will.
The kids’ sleep puzzle
At Well Spoken we use a ‘road map’ to decide how we can address sleep problems irrespective of the cause and severity. Here is a simplified version of the Well Spoken roadmap we use to guide our clinical decision making and discussions with parents, including evaluating whether medical, dental or allied health or whether improving upper airway health and ‘fitness’ is necessary.
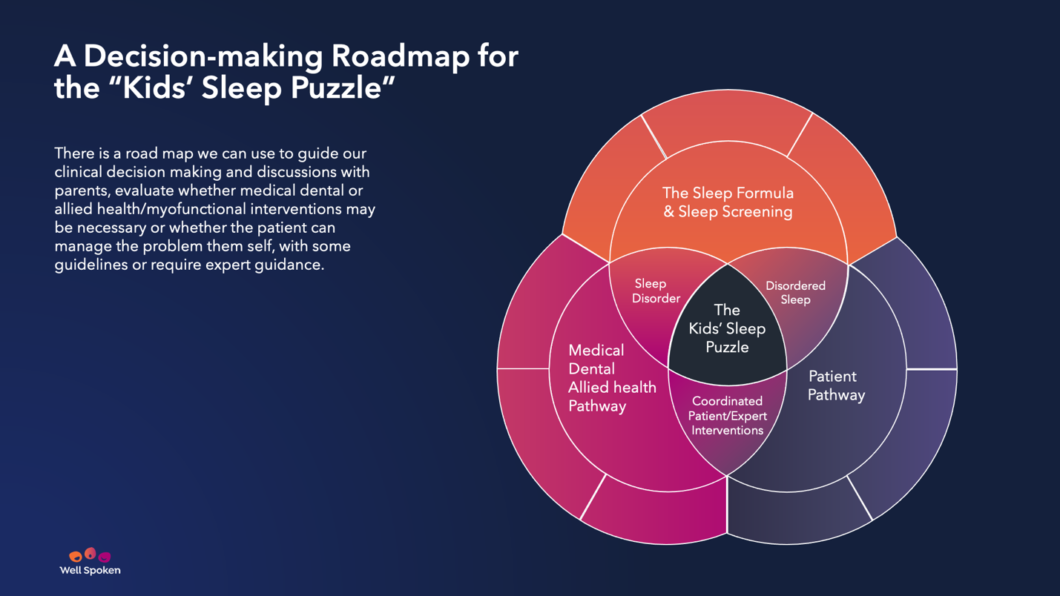
The sleep formula & sleep screening
At Well Spoken we start by talking about the good sleep formula i.e. the quantity and quality of sleep required for great sleep every night. Sleep screening then provides us with a way to understand what is happening right now. This means parents fil out questionnaires and capture short videos and photos of their child sleeping so we can understand exactly what is happening during sleep.
The patient pathway
Once we have sleep screening results Well Spoken provides patient education to improve, sleep health practices, optimising environment, behavior & routines, and tips for upper-airway health like keeping the nose clear, managing allergies, middle ear effusion, food intolerances or reflux.
Medical, dental and allied health treatment pathway
We also need to know if other medical or dental professionals need to be involved in a child’s care. Our questionnaires and detailed upper airway assessment allow us to understand whether a patient requires expert medical, dental or allied health support Together with parents we need to decide next steps:
- When: Triage the urgency
- Who: Decide who needs to be involved and make necessary referral/s
- What: Create a detailed ‘upper airway’ treatment plan for children with sleep-breathing issues.
So, in conclusion, sleep brilliantly is important. There is much parents can do all on their own at home to improve sleep environment and establish healthy sleep practices. Sometimes, expert medical and dental and allied health experts may be required to help improve sleep efficiency. At Well Spoken we say treat as early as possible, don’t wait.
Thanks so much for tuning in.



